Connect With Us
Blog
Foot Problems That Can Lead to Ongoing Pain
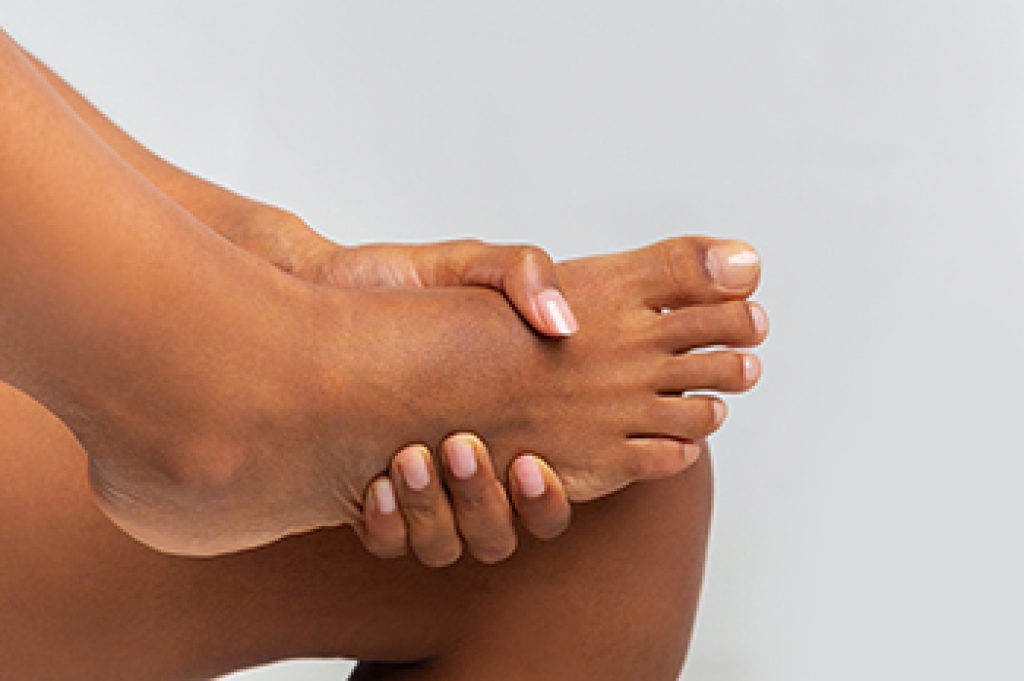
Foot pain can come from several conditions, including Achilles tendinitis, bone spurs, and bunions, each affecting the foot in different ways. Pain from Achilles tendinitis is often felt at the back of the heel and may cause stiffness, especially after rest or activity. Bone spurs are bony growths that can develop on the heel or joints, sometimes leading to irritation and discomfort with walking. Bunions appear as a bony bump at the base of the big toe, often causing redness, swelling, and difficulty wearing shoes. These conditions may result from repetitive stress, improper footwear, inherited foot structure, or aging. A podiatrist can evaluate the source of pain through examination and imaging to create a treatment plan tailored to the condition. Care options include supportive footwear, custom orthotics, and targeted exercises to relieve strain and improve function. Early treatment can help reduce pain and prevent progression. If you have foot pain, it is suggested that you make an appointment with a podiatrist for a diagnosis and treatment plan.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Jeffrey L. Bober, DPM from Maryland. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact our office located in Glen Burnie, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Managing Toe Pain

Toe joint pain can make walking uncomfortabl,e and may interfere with daily activities. It often develops from arthritis, overuse, injury, or structural problems in the foot. The pain may be felt in the big toe or smaller toes, and can result in stiffness, swelling, or a deep aching sensation. Some people notice redness, warmth, or a reduced ability to bend the toe, especially during push off when walking. In certain cases, sharp or sudden pain in the big toe joint may be related to gout. The joint may appear enlarged or tender, and discomfort can worsen with activity or pressure from footwear. A podiatrist can evaluate joint movement, foot structure, and possible underlying causes through an examination and imaging tests. Relief options can include wearing supportive footwear, custom orthotics, anti-inflammatory care, and targeted exercises to maintain mobility. If you have persistent toe joint pain, it is suggested that you schedule an appointment with a podiatrist for appropriate relief and treatment solutions.
Toe pain can disrupt your daily activities. If you have any concerns, contact Jeffrey L. Bober, DPM of Maryland. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Causes Toe Pain?
Most severe toe pain is caused due to a sports injury, trauma from dropping something heavy on the toe, or bumping into something rigid. Other problems can develop over time for various reasons.
Toe pain can be caused by one or more ailments. The most common include:
- Trauma
- Sports injury
- Wearing shoes that are too tight
- Arthritis
- Gout
- Corns and calluses
- Hammertoe
- Bunions
- Blisters
- Ingrown toenails
- Sprains
- Fractures (broken bones)
- Dislocations
When to See a Podiatrist
- Severe pain
- Persistent pain that lasts more than a week
- Signs of infection
- Continued swelling
- Pain that prevents walking
Diagnosis
In many cases the cause of toe pain is obvious, but in others, a podiatrist may want to use more advanced methods to determine the problem. These can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatments for toe pain and injuries vary and may include shoe inserts, padding, taping, medicines, injections, and in some cases, surgery. If you believe that you have broken a toe, please see a podiatrist as soon as possible.
If you have any questions please contact our office located in Glen Burnie, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Fracture Blisters on the Foot

Fracture blisters are fluid-filled skin lesions that develop on the foot after a bone fracture, caused by intense swelling and pressure that disrupts the layers of the skin, often appearing clear or filled with blood. These blisters are typically accompanied by pain, swelling, and a feeling of tightness in the affected area, and may increase the risk of infection, if not treated promptly and properly. Common causes include traumatic injuries such as falls, accidents, or sports-related impacts, while risk factors include severe swelling, poor circulation, and delayed medical attention. A podiatrist can assess the injury, protect the skin, and support proper healing. If you notice blistering after a foot injury, it is strongly suggested that you consult a podiatrist who can offer effective relief and treatment solutions.
Blisters may appear as a single bubble or in a cluster. They can cause a lot of pain and may be filled with pus, blood, or watery serum. If your feet are hurting, contact Jeffrey L. Bober, DPM of Maryland. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters are often the result of friction. This happens due to the constant rubbing from shoes, which can lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
Symptoms
(Blister symptoms may vary depending on what is causing them)
- Bubble of skin filled with fluid
- Redness
- Moderate to severe pain
- Itching
Prevention & Treatment
In order to prevent blisters, you should be sure to wear comfortable shoes with socks that cushion your feet and absorb sweat. Breaking a blister open may increase your chances of developing an infection. However, if your blister breaks, you should wash the area with soap and water immediately and then apply a bandage to the affected area. If your blisters cause severe pain it is important that you call your podiatrist right away.
If you have any questions, please feel free to contact our office located in Glen Burnie, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Understanding Corns and Calluses and How They Are Treated
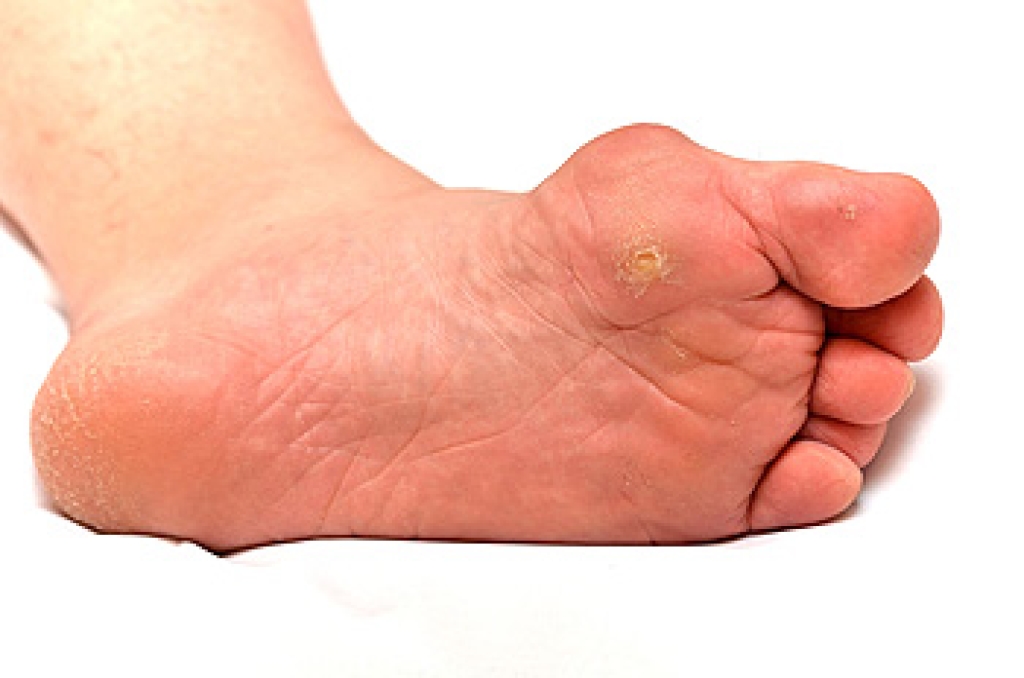
Corns and calluses are thickened areas of skin that develop from repeated pressure or friction. A corn is a small, focused area of hardened skin that often forms on or between toes and may feel painful due to its deeper core. A callus is a larger, flatter area that usually develops on the bottom of the foot, and may feel rough rather than painful. Treatment begins by reducing the source of pressure, which may include wearing better fitting shoes, padding, or custom orthotics. A podiatrist can safely trim thickened skin to relieve discomfort and improve function. In some cases, underlying foot structure or walking patterns need to be addressed to prevent the return of these problems. Avoid cutting these areas at home, as this can lead to injury or infection. If you have persistent thickened skin or pain on your feet, it is suggested that you see a podiatrist for a proper diagnosis and appropriate care.
If you have any concerns regarding your feet and ankles, contact Jeffrey L. Bober, DPM of Maryland. Our doctor will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
- Well-fitting socks
- Comfortable shoes that are not tight around your foot
- Shoes that offer support
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Our doctor to determine the best treatment option for your case of corns.
If you have any questions, please feel free to contact our office located in Glen Burnie, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blog Archives
- 2026
- 2025
- 2024
- 2023
- 2022
- 2021

