Connect With Us
Blog
Plantar Fibroma and Fibromatosis Management Options
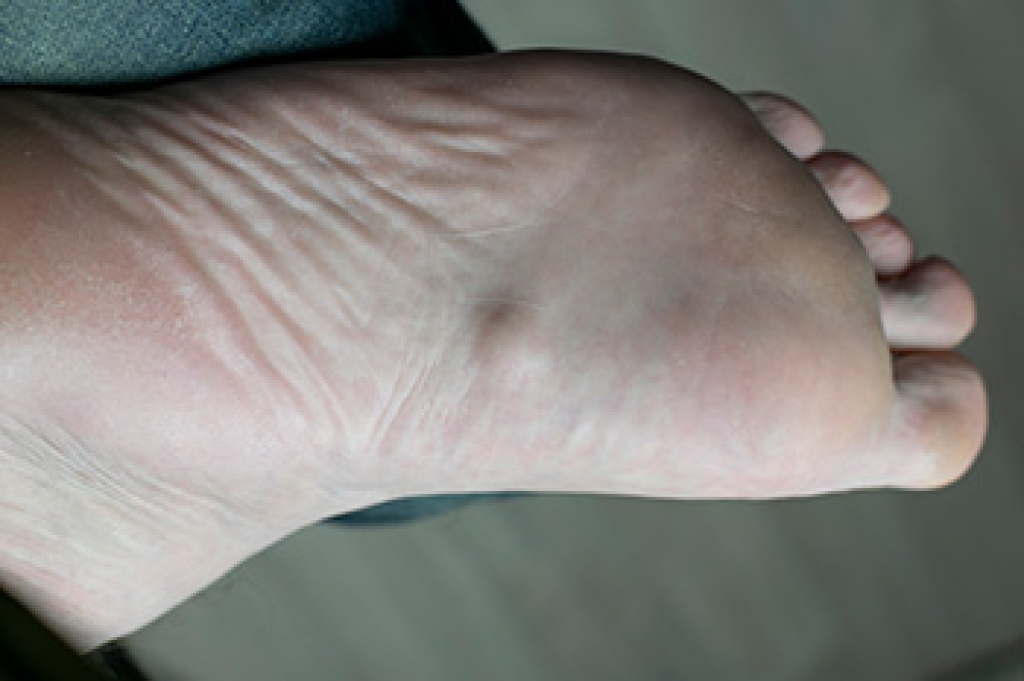
A plantar fibroma is a single benign lump that develops within the plantar fascia, the thick band of tissue along the bottom of the foot. Plantar fibromatosis refers to a more extensive condition in which multiple fibromas form and may gradually enlarge or spread. Both can cause localized pain, pressure with walking, and discomfort when standing for long periods, although fibromatosis is often more persistent and challenging to manage. Treatment focuses on reducing pressure and irritation. Custom orthotics, padding, and wearing supportive footwear help offload the affected area. Stretching and anti-inflammatory measures may ease symptoms. In some cases, targeted injections or other conservative therapies are considered. Surgery is approached cautiously, especially with fibromatosis, due to recurrence risk and scar tissue development. When ongoing arch pain or lumps interfere with daily activities, it is suggested that you obtain an evaluation by a podiatrist who can guide appropriate management and treatment.
A plantar fibroma may disrupt your daily activities. If you have any concerns, contact Jeffrey L. Bober, DPM of Maryland. Our doctor can provide the care you need to keep you pain-free and on your feet.
Plantar Fibroma
A plantar fibroma is a fibrous knot in the arch of the foot. It is embedded in the plantar fascia which is a band of tissue that extends from the heel to the toes along the bottom of the foot. There can be multiple plantar fibromas in the feet at the same time. There are no known causes for this condition. If you have a plantar fibroma, there will be a bump in the arch of your foot that cannot be missed. Any associated pain is most often due to a shoe rubbing against the nodule. Non-surgical options, such as steroid injections, physical therapy, and orthotics should be tried first. Surgery is a last resort and is the only thing that will remove a plantar fibroma entirely. Consult with a podiatrist for a proper diagnosis and to determine the treatment regimen that is right for you.
What Causes a Plantar Fibroma?
While there are no specific causes identified, a plantar fibroma can possibly come from genetic predisposition or the formation of scar tissue that forms from healing the tears in the plantar fascia.
What Are the Symptoms of a Plantar Fibroma?
There will be a noticeable lump in the arch of the foot that may or may not cause pain. If pain is felt, it is typically because a shoe is rubbing up against the lump or when walking or standing barefoot.
Treatment and Prevention
A plantar fibroma will not disappear without treatment, but it can get smaller and be a non-issue. If pain persists, a podiatrist examines the foot and when the arch of the foot is pressed, pain can be felt down to the toes. An MRI or biopsy might be performed to help diagnose or evaluate the plantar fibroma. The following non-surgical options are generally enough to reduce the size and pain of these nodules:
- Steroid injections
- Orthotics
- Physical therapy to help apply anti-inflammatory creams on the bump
Surgery is considered if the mass increases in size and the patient continues to feel pain after non-surgical methods are tried.
If you have any questions, please feel free to contact our office located in Glen Burnie, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Heel Spur Exercises for Pain Relief

Heel spurs are bony growths on the heel that often cause sharp pain, tenderness, and inflammation, especially while walking or standing. Symptoms include stabbing pain in the heel, swelling, or discomfort after rest. Effective exercises can reduce pain and improve foot function. These can include the foot flex, which involves bending the foot upward and downward to stretch and strengthen the plantar fascia, the thick band of tissue on the sole of the foot. Calf stretches on a step help lengthen the calf muscles and Achilles tendon, relieving tension on the heel. Additionally, the toe towel grab strengthens foot muscles by picking up a towel with the toes. A podiatrist can evaluate heel pain, and recommend proper stretches. If you have heel pain, it is suggested that you consult a podiatrist who can accurately diagnose what may be going on, and start you on a personalized plan for relief and improved foot health.
Exercising your feet regularly with the proper foot wear is a great way to prevent injuries and build strength. If you have any concerns about your feet, contact Jeffrey L. Bober, DPM from Maryland. Our doctor can provide the care you need to keep you pain-free and on your feet.
Exercise for Your Feet
Exercise for your feet can help you gain strength, mobility and flexibility in your feet. They say that strengthening your feet can be just as rewarding as strengthening another part of the body. Your feet are very important, and we often forget about them in our daily tasks. But it is because of our feet that are we able to get going and do what we need to. For those of us fortunate enough to not have any foot problems, it is an important gesture to take care of them to ensure good health in the long run.
Some foot health exercises can include ankle pumps, tip-toeing, toe rises, lifting off the floor doing reps and sets, and flexing the toes. It is best to speak with Our doctor to determine an appropriate regimen for your needs. Everyone’s needs and bodies are different, and the activities required to maintain strength in the feet vary from individual to individual.
Once you get into a routine of doing regular exercise, you may notice a difference in your feet and how strong they may become.
If you have any questions, please feel free to contact our office located in Glen Burnie, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Powering Through Pain in the Achilles Tendon

Athletes who rely on running, jumping, or sudden changes in direction may experience pain in the Achilles tendon, the strong band connecting the calf muscles to the heel. This condition often appears as swelling or thickening along the back of the heel and can feel stiff, tender, or sharp during activity. Common causes include overuse, sudden increases in training intensity, tight calf muscles, or improper footwear. Symptoms may worsen with activity and improve with rest, yet persistent pain can limit performance. A podiatrist begins with a detailed exam and imaging when needed to assess tendon integrity and rule out tears. Treatment may include stretching and strengthening exercises to restore flexibility and support, orthotics or heel lifts to reduce strain, and activity modification. Early intervention can prevent further injury and speed recovery. If you have Achilles tendon pain, it is suggested that you make an appointment with a podiatrist.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Jeffrey L. Bober, DPM of Maryland. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our office located in Glen Burnie, MD . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Diagnosing and Treating an Ankle Fracture

An ankle fracture occurs when one or more bones forming the ankle joint break, often after a fall, misstep, sports injury, or accident. Diagnosis begins with a careful clinical exam to assess pain, swelling, bruising, and the ability to bear weight. Imaging plays an important role. X-rays are commonly used to confirm a break and determine alignment, while advanced imaging may be recommended if the injury is complex or involves surrounding structures. Treatment depends on the type, location, and stability of the fracture. Stable breaks may be managed with immobilization using a boot or cast, along with limited weight-bearing. More severe injuries may require realignment or surgical repair to restore joint stability. Targeted exercise is an important part of recovery and helps rebuild strength, mobility, and balance. Prompt care reduces the risk of long-term stiffness, arthritis, or instability. If you have sustained an ankle injury that is causing significant pain, swelling, or difficulty walking, it is suggested that you seek prompt evaluation by a podiatrist.
test
Blog Archives
- 2026
- 2025
- 2024
- 2023
- 2022
- 2021

